The National Institute for Health and Care Excellence (NICE) provides national guidance and advice to improve health and social care, and whose guidelines are used across the NHS. NICE are developing a new Interventional Procedures Guidance which looking at using Deep brain stimulation (DBS) for obsessive-compulsive disorder.
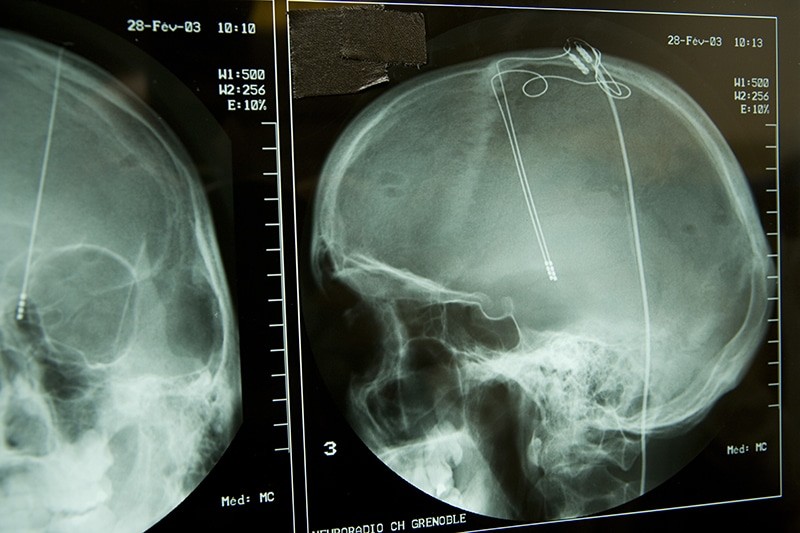
Obsessive-compulsive disorder is a mental health condition in which a person has obsessive thoughts (repeated, unwanted and unpleasant thoughts, images or urges). The person feels the need to carry out repetitive behaviours (compulsive), to try to relieve the unpleasant feelings brought on by the obsessive thoughts. Symptoms can be distressing and interfere with normal life. In this procedure, an electrode is put into the brain and connected to a wire that is tunnelled under the skin behind the ear and down the neck. The wire is attached to an electrical stimulator that is put under the skin on the chest. The aim is to reduce the obsessive-compulsive thoughts and behaviours.
NICE are inviting OCD-UK members and service-users views on the procedure, these are the three important questions we are asking people with OCD (and/or carers) to comment on about the potential use of DBS for OCD.
- What do patients (or carers) think the advantages of the procedure or operation are?
- What do patients (or carers) think the disadvantages of the procedure or operation are?
- Are there any groups of patients who might benefit either more or less from the procedure or operation than others? If so, please describe them and explain why.
Please send your comments by email to office@ocduk.org. All submissions will be submitted to NICE by us anonymously.
Please submit to us by 5pm on Friday 6th December 2019.