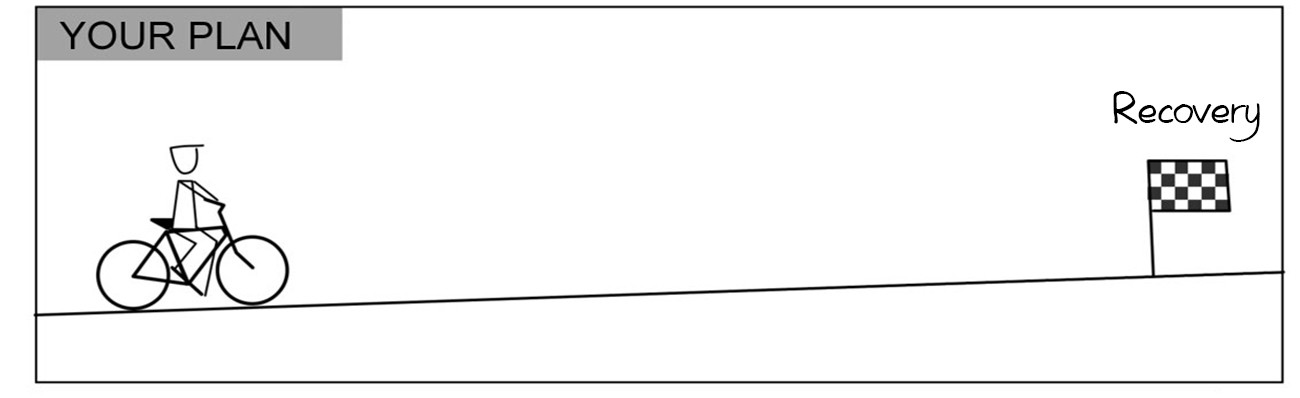
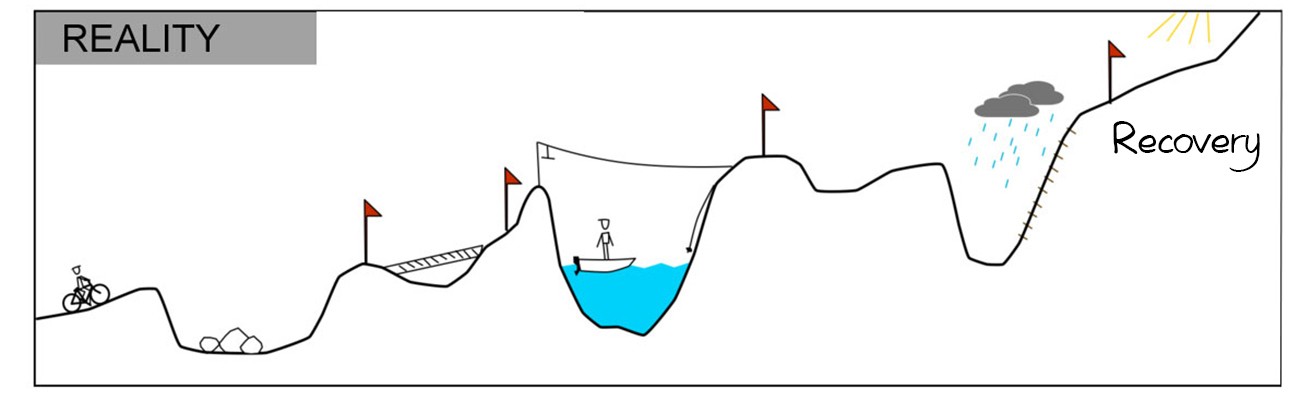
When we first enter therapy, it’s natural to expect after hearing stories of people recovering from OCD, our own recovery journey to be relatively straight forward, if not slightly uphill.
But the reality is in many cases it’s likely to be very different, because overcoming OCD requires lots of hard work, and has some challenging obstacles. On occasions we may have to go backwards to find another route over an obstacle to move forwards again.
This is why the importance of working at therapy is the one key message we want people to take away from this website, well, that and the fact that the recovery destination is actually an achievable place to reach.
The fact is, it’s US that have to do most of the hard work to get there, our therapist is a guide and will be there to help us through those difficult challenges, but ultimately it’s us that have to push ourselves forward.
Whilst we know Cognitive Behavioural Therapy (CBT)
helps many people overcome OCD, too many people fall into the trap of becoming complacent, believing that the therapist and the therapy are going to do all the work, so we want to throw a few of those common myths out there to ensure there is no misunderstanding about our role in therapy.
The unhelpful beliefs about therapy listed below have all been used over time, probably by many of us here at OCD-UK and are worth exploring.
- Therapy is once a week in the therapists office
- We will be better at the end of the 10/12 week therapy course
- The therapist will do most of the work
- I have had CBT, but it did not work for me, so it won’t work at all
Therapy is once a week in the therapists office.
Whilst yes, the actual therapy appointment will be weekly (or bi-weekly) in most cases, the fact is, therapy SHOULD happen throughout the week, not just during sessions. In fact, homework is set by the therapist to enable the patient to work at therapy during the week, so in reality you could suggest that the ‘real’ therapy actually happens away from the therapist’s office.
But don’t worry if you can’t do that at first, it takes time to become your own therapist.
We will be better at the end of the 10-18 week therapy course.
Now wouldn’t that be lovely, and of course it’s not impossible, but the reality for most of us is that whilst we will have improved, we will still have OCD, so it’s important we work at applying therapeutic techniques long after therapy.
If the therapist has done their job correctly, then you should feel empowered to become your own therapist, and start applying therapeutic techniques throughout your day, at home and at work, and you should be engaging in uphill challenges every day, until you’re powering through them Chris Froome style.
The therapist will do most of the work.
Attending therapy, and expecting to have an easy ride, with the therapist on front of a tandem, doing all the hard work for you, whilst appealing, is simply not realistic or sustainable to empower you to reach your recovery destination, and to maintain your place at that location.
The therapist is there to guide you, support you like a team principle and even be your domestique (another cycling term – a rider who works for the benefit of the team leader), but ultimately if you want to reach your destination, we need to acknowledge the importance of working at it.
I have had CBT, but it did not work for me, so it won’t work at all
Chris Froome did not win the Tour de France without first training hard, and recognising the importance of working at it with many, many bike races before he conquered the tour. Therapy is exactly the same, sometimes we have to enter different races (course of therapy), perhaps with a different team (therapist) who are better equipped (knowledgeable about OCD) to help us reach our recovery destination.
Summary
The importance of working at therapy should not be underestimated, whilst working at it doesn’t guarantee success, not working at therapy does guarantee failure!
Throughout the website we refer to CBT as a talking therapy, which it is, but it shouldn’t be viewed as just a talking therapy, to quote psychologist, Dr Lucy Oldfield,
CBT isn’t a talking therapy, it’s a doing therapy.
What to read next: