As you already know, the treatment OCD-UK recommend is Cognitive Behavioural Therapy (CBT), which is also recommended by the NICE Guidelines for the treatment of OCD. But, the NICE Guidelines don’t actually cover Scotland, although generally most health practitioners will be open to accepting NICE recommendations outside of England and Wales.
As you already know, the treatment OCD-UK recommend is Cognitive Behavioural Therapy (CBT), which is also recommended by the NICE Guidelines for the treatment of OCD. But, the NICE Guidelines don’t actually cover Scotland, although generally most health practitioners will be open to accepting NICE recommendations outside of England and Wales.
Scotland does actually have its own version, called SIGN, which stands for Scottish Intercollegiate Guidelines Network. Sign was formed in 1993, and their objective is to improve the quality of health care for patients in Scotland by reducing variation in practice and outcome, through the development and dissemination of national clinical guidelines containing recommendations for effective practice, based on current evidence. Basically, it operates very similarly to NICE, however, at this time SIGN do not have a set of guidelines to cover Obsessive-Compulsive Disorder.
NHS Scotland do have their own national health information service, which is called NHS Inform, which aims to provide Scottish residents with accurate and relevant information to help them make informed decisions about their own health. In their advice for Obsessive-Compulsive Disorder, NHS Inform follows NICE and recommends CBT as the main treatment for OCD.
But as with the rest of Great Britain, how people access CBT through the NHS in Scotland can be a complex, confusing and often challenging pathway. The process for accessing NHS treatment is not too dissimilar as of that in England, but the main difference is the fact there is no IAPT service, and therefore the ability to self-refer is not currently available in all areas of Scotland (at the time of writing). You may wish to check with your local NHS board if they currently offer mental health self-referral services similar to those offered by IAPT service in England which offer Cognitive Behavioural Therapy (CBT).
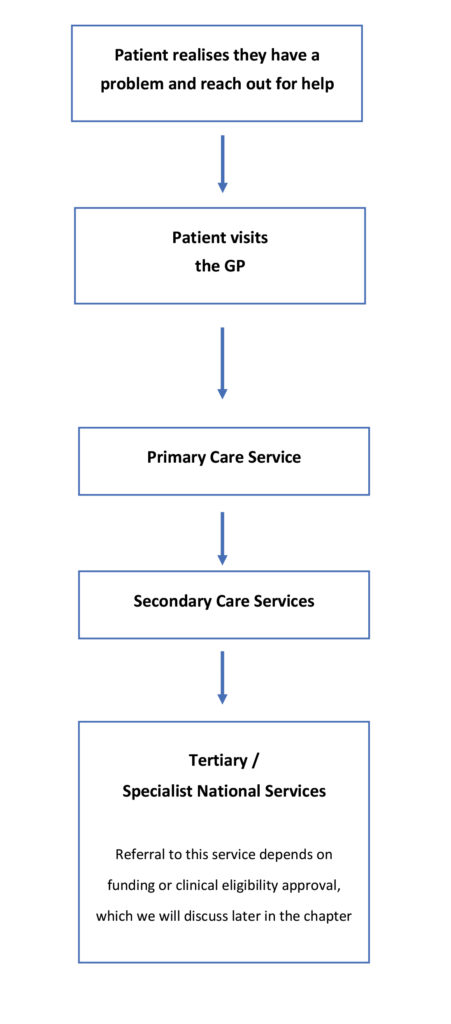
The illustration below is a basic outline of the route patients usually take in accessing OCD treatment, starting with their GP (unless a self-refer option is available within their local health board) .
Mental health treatment across Scotland is provided by local NHS boards, unlike in England where services are provided by a Clinical Commissioning Group (CCG).
There are fourteen local NHS boards in Scotland, and they are responsible for the protection and improvement of their population’s health and for the delivery of frontline healthcare services, such as mental health services. Those fourteen NHS boards are: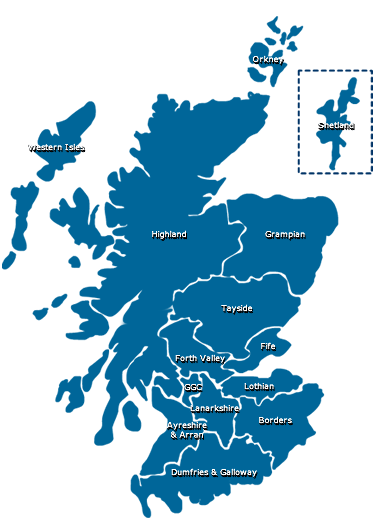
- NHS Ayrshire and Arran
- NHS Borders
- NHS Dumfries and Galloway
- NHS Fife
- NHS Forth Valley
- NHS Grampian
- NHS Greater Glasgow and Clyde
- NHS Highland
- NHS Lanarkshire
- NHS Lothian
- NHS Orkney
- NHS Shetland
- NHS Tayside
- NHS Western Isles
The illustration above is a fairly typical route for patients in Scotland to access treatment, but there may be some local variations within each service.
Route 1 – GP > Primary Care
Despite the breakthroughs in awareness, understanding and treatment of OCD, many GPs and mental health professionals still do not recognise the symptoms of the disorder or even know how to correctly treat it. Therefore, we encourage you to be specific and clear when telling your GP that you “believe you may (or do) have OCD and would like to be referred for Cognitive Behavioural Therapy (CBT)”.
Sometimes people are worried about opening up about their OCD, so if you’re reticent about opening up to your GP, we have created a GP Ice-Breaker printout to help you during that first visit, which can also be used when you first see a mental health professional.
Although medication is not recommended as a sole treatment method for OCD, in practice many people will be offered it when on long waiting lists for therapy. If this happens, it is your choice whether to accept the medication, some people find it helps keep them afloat whilst waiting for therapy.
The GP should refer you for therapy (CBT), usually to the local community mental health team (CMHT). At this point the patient is in the hands of the local health board in terms of treatment waiting times.
Before accessing any kind of treatment it’s worth considering what you can do to prepare for therapy, and also review some of the potential barriers for treatment.
If you’re a parent of a child with OCD the same process applies, other than instead of adult services, the GP will refer your child to local CAMHS services (pronounced CAMS), with CAMHS standing for Child and Adolescent Mental Health Service.
For many people with OCD, the level of treatment and support they receive through their local community mental health service will be sufficient and allow them to make progress towards recovery. Some however may need more therapy over a longer period, perhaps a little more intensive, and therefore are referred to local secondary care services.
Secondary Care > Specialist Services
Accessing secondary care services requires either a referral from a GP or in some cases, the primary care service will refer you straight to the relevant service. This can mean a break in treatment between services. Sometimes a GP may feel a patient will benefit more from this level of treatment and refer you directly to secondary care services.
Treatment within secondary care services will not be dissimilar from what you’ve experienced previously, the key difference being that these are usually consultant-led services, which include psychology and psychiatry. They may offer additional services like prolonged therapy with a clinical psychologist, medication reviews with a psychiatrist, access to training and other facilities. The course of treatment is likely to be less time restricted than in primary care, allowing patients more time to work on their problems.
For a small number of people, local services may not be enough to help them make sufficient progress and may benefit from a referral to a specialist OCD service, sometimes called tertiary care.
(Tertiary) National Specialist Services
In Scotland there is a specialist service for the treatment of OCD based in Dundee called the Advanced Intervention Service (AIS). The AIS clinic has a national contract with NHS Scotland, that means patients located anywhere in Scotland can be referred to the clinic without treatment funding needing to be approved by their local NHS Board (although patients usually have to been treated for OCD by their local NHS Board previously to be eligible). Patients in Scotland can also access the specialist treatment clinics in England, but referral to those requires local NHS Board funding approval first.
We go into details about all those specialist OCD clinics, where they’re located and what they offer later in this section.
What to read next: